

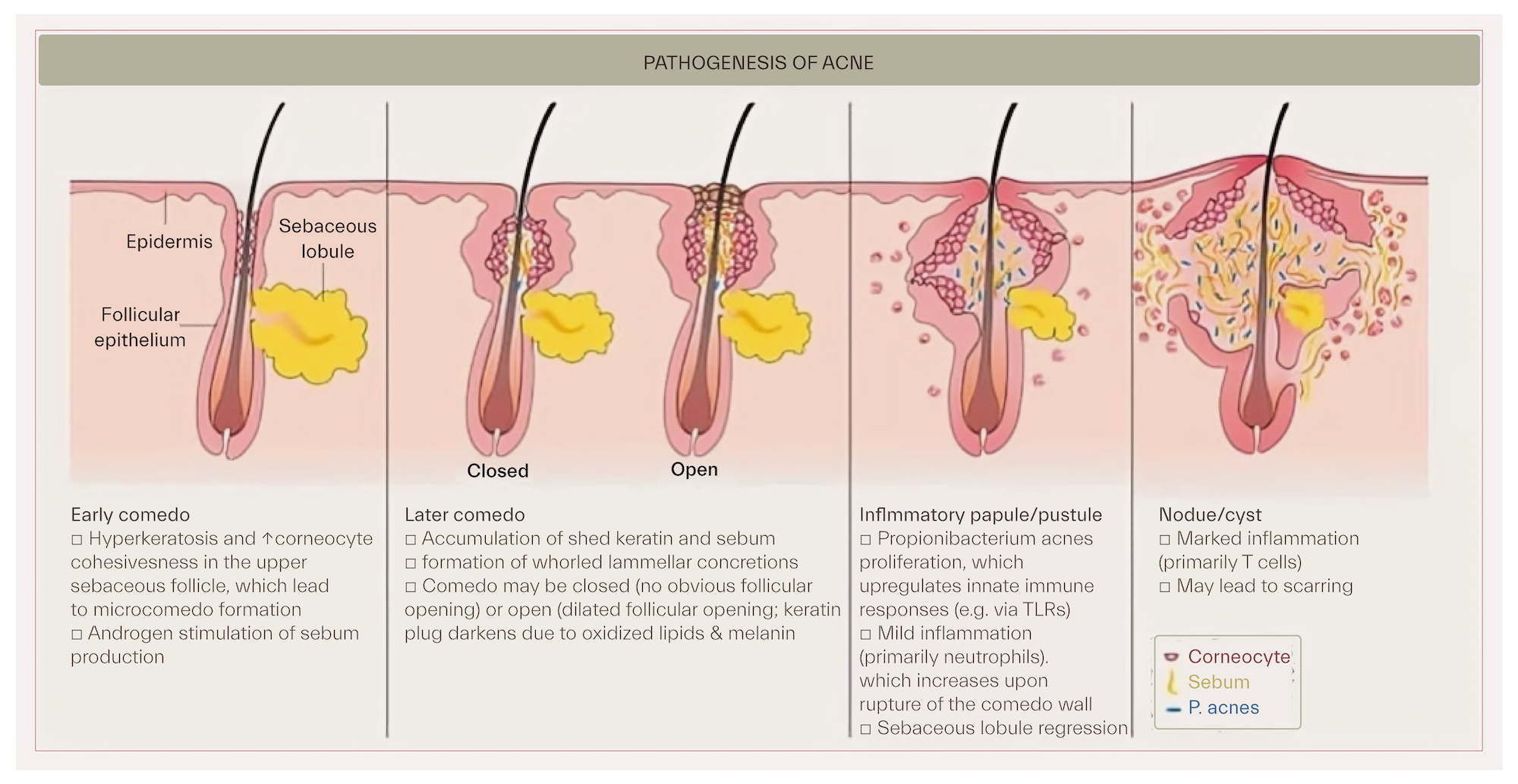
With most prescription types for comedonal acne treatment, results may not be seen for 6 to 8 weeks, and the skin is likely to get worse before it gets better. No single approach is full proof in treatment of acne and clinical guidelines which represent an epitome of generalities, must be individualized. Despite lack of high strength of recommendation in the guidelines, acne skin care prevails far more widely, grows in substantiation and becomes standard of care as an adjunct in treatment of exacerbations of all stages as well as maintenance treatment of acne vulgaris.
According to guidelines, retinoids are mainstay of treatment for comedonal acne while benzoyl peroxide and azelaic acid are indicated with low strength of recommendation. Retinoids as well as benzoyl peroxide regardless of concentration are highly irritating to the skin with predilection to precipitate atopic dermatitis in some individuals. On the other hand, while alteration of skin lipids and sebum composition account for severity of lesions, neither retioids nor benzoyl peroxide have been found to disburden this culprit.
Comedonal acne treatment is mainly directed toward a maintenance skin care for acne to regulate sebum and no antibiotic use
Provision of depleted lipids and associated proteins, lost in part due to the disease and in part due to the use of treatment agents, to overzealous hyperfunctional sebaceous unit has been often overlooked, if not entirely left to oblivion in the present treatment protocols. Built upon this principle, an skin care tailored for acne prone skin finds its way to management regimens not only in maintenance but concurrent with modalities used in exacerbation.
Evidence based skin care for comedonal acne treatment aim to dry up the excess oil, kill bacteria, promote shedding of dead skin cells by which helps to treat comedones . Over-the-counter acne lotions are generally the first remedy acne patients resort to and contain benzoyl peroxide, sulfur, resorcinol or salicylic acid as their active ingredient. These products can be helpful for very mild forms of acne lesions. Topical acne treatment modalities remain the primary, unmatched and sole option in multitude of acne patients and constitute part of long term objectives for acne therapy for those who do not show adequate response to oral treatments. Failure of response to OTC products warrants seeking treatment from a family doctor or a dermatologist to receive prescription lotion.
Tretinoin treatment (Retin-A) and adapalene are topical prescription products derived from vitamin A. They work at the skin pore level to prevent plug formation. A number of topical antibiotics also are available, used in conjunction with retinoids and benzoyl peroxide to treat moderate acne. They work by disburdenin excess skin bacteria which cause acne, propionibacterium acnes and staphylococcus species. Often, a combination of such products is required to achieve optimal results.
Antibiotics: For moderate to severe acne forms such as nodules and cysts, prescription oral antibiotics may be needed to reduce bacteria and temper inflammation while isotretinoid is warranted in certain patient population. Antibiotics may be continued for months and often need to use them in combination with topical products such as retinoids and benzoyl perpoxide. Acne spots and other pigmentations/discolorations are another concern of many patients suffering acne. Acne treatment procedures, such as light therapy, steriod injection, chemical peels are considered as open options with low level of recommendation.
Comedonal acne is presented with papules and limited pustules, indicative of restricted inflammation
Guidelines recommend use of multiple agents in control of acne of various severity. This principle applies to mild acne, treated in large by benzoyl pleroxide and topical retinoids alone or in combination, other topical agents, clindamycin, erythromycin, may be used in combination therapy of mild acne. Combination therapy has not been implemented central to comedonal acne treatment, however, evidence based acne skin care, which employ various full proof ingredients known to be effective in control of comedones, is growing in acceptance and exercise. Topical retinoid and salicylic acid are most well known comedolytic agents utilized in comedonal acne. In addition, azelaic acid and benzyoyl peroxide are mildly comedolytic and hence of benefit in treating comedones.>
First line treatment for moderate acne vulgaris includes a combination of benzoyl peroxide and a topical or systemic antibiotic, clindamycin or erythromycin, with or without a topical retinoid. In severe disease, oral antibiotics are used in combination with topical retinoid and/or benzoyl peroxide. Alternatively, oral isotretinoin could be started in selected patients. AAFP recommends use of oral tetracycline as a first choice antibiotic in moderate to severe acne, however, its adverse effects casts caution on its use especially on continuous or long term use. Topical or oral antibiotic may not be used alone for the concern regarding antibiotic resistance.
Cystic acne treatment generally employs multiple modalities to get rid of deep cysts and nodules. Amid oral acne treatments, Isotretinoin (Accutane) is an effective medication available for severe forms such as nodulocystic acne or acne conglobata that do not respond to other acne treatment options. Patients who take isotretinoin require close monitoring by a dermatologist because of the possibility of severe side effects such as allergic reaction (inflammation of face and tongue) blurred vision, dryness of the vision and etc. Pregnancy, especially during the early stages is a contraindication for certain oral prescription types acne treatment.
Oral contraceptives. Oral contraceptives, including a combination of norgestimate and ethinyl estradiol (Ortho-Cyclen, Ortho Tri-Cyclen), have been shown to improve acne in women. Oral contraceptives may cause other side effects that may be taking into account before administration. Evidence comparing efficacy of oral conctraceptive versus oral antibiotics are either lacking or conflicting.
Cosmetic surgery. Cosmetic surgery is often viewed as a high cost option to diminish scars left by inflammatory acne. Procedures include peeling away damaged skin with chemicals or by freezing it, dermabrasion and laser resurfacing. Peeling procedures eliminate superficial facial scarring. Dermabrasion, which is usually reserved for more severe scars, involves removing the top layers of skin with a rapidly rotating wire brush. Laser resurfacing involves using short pulses of intense light to remove the outer layer of your skin. If your skin tends to form scar tissue, these procedures can make your complexion worse.
Control of whiteheads or closed comedones and blackheads or open comedones can be achieved in most cases with regular use of maintenance skin care , a wholesome diet and adherence to a good hygiene and discussed below in more detail. Prevention is bound to far greater outcomes as it aids to keep relapses at bay and less frequent use of antibiotics which pose a concern with bacterial resistance.
Prevention is the regular use of appropriate therapeutic agents to ensure that acne remains in remission. Topical comedonal acne treatment is the mainstay of maintenance therapy. A number of topical therapeutic options have been selected, including alpha hydroxy acids such as glycolic acid and beta hydroxy acids, salicylic acid most notorious, benzoyl peroxide, and azelaic acid are number of agents with proven clinical efficacy which can effectively harness a relpase which may require an oral treatment.
Selection of topical agents is mainly based on a number of criteria. First, efficacy in treating microcomedones, which are the precursor lesions for both comedones and inflammatory acne lesions. Second is tolerability, due to the need for application of a topical agent to a broader epidermal layer; such as whole face as opposed to on the spot application and other properties that may enhance adherence. Patients tend to be more motivated to use agents that are easily integrated into their lifestyles and that have potential “skin-repairing” properties, which again cast approbation on use of an skin care regimen which can effectively treat acne.
Skin-Repairing effects of maintenance comedonal acne treatment is another aspect of any protocol which adds more heft to its efficiency. Acne causes disruptions in the epidermal barrier. Such barrier defects can be associated with transepidermal water loss and an increased potential for exposure to environmental irritants. Topical agents with skin repairing properties such as retinoids or salicylic acid in preparations such as serums or lotions as adjuvants to oral modalities can maintain epidermal integrity and probe transepidermal dehydration. This aspect of treatment is addressed in a skin care for acne and enhance patient compliance by improving overall skin appearance and may be continued in the absence of visible lesions.
Acne scars especially are sequeles that acne patients have to deal with even after skin clarification and cause of great concern for this patient population. Available procedures for improving appearance of acne scars may be rather costly. Skin care serums, serum for acne scars, as more effective vehicles as opposed to other preparations such as lotions or creams seem to be a viable option with skin resurfacing outcomes comparable with office procedures.
Wash problem areas with a gentle non-alcoholic, low pH cleanser. For their alkaline pH, much higher than acid mantle, soaps are not recommended since they can stimulate the skin to secrete more oil and interfere with the cutaneous microflora. Excessive washing and use of astringents, containing alcohol, generally may not be helpful in comedonal acne treatment because they tend to overdry and irritate the skin, which can aggravate whiteheads and blackheads by provoking sebaceous glands to generate more oils to combat dry skin. Products such as facial scrubs and scrubbing also can irritate skin through mechanical stimulation of the skin. Scrubbing the skin may be avoided.
Avoid irritants. You should avoid oily or greasy cosmetics, sunscreens, hair- styling products or acne concealers. Use of products labeled “water-based” or “noncomedogenic” or “oil free” does not guarantee their safety to your skin. Unlike a common disbelief, use of certain oily products containing gamma linolenic acid, alpha linolenic acid, omega 3 fatty acids can yield favorable results for their attenuation of inflammatory processes as well as fighting bacterial pathogens implicated in acne. These oils can regulate sebaceous overactivity , reduce oiliness of the skin and be utilized for effective comedonal acne treatment. Any skin care for acne prone skin should include a elemental sun protection, in part, due to formation of squalene peroxide, a by-product of UV irradiation in skin, which is proinflammatory and deleterious to comedonal acne. Besides, use of various modalities in management of comedones such as retionids, benzoyl peroxide, azelaic acid, tetracylcine, makes skin more photosensitive and vulnerable to sunburn.
The significance of stress, a well-recognized impetus contributing to acne, ought to be emphasized and stress management strategies are key in control of the disease. Sleep hygiene and regular exercise are well supported in coping with daily stress and could be of great benefit.
Mechanical stimulation of blemishes may lead to infection or scar tissue. Sleeping in a way that cause face to touch a pillow may cause acne. Avoid using tweezers or any other removal objects. Styling hair products can contribute to blemishes on the forehead. Caution should be exercise what touches the face while it is important to keep the hair clean and off the face and avoid resting the hands or objects on the affected areas. Sweating in tight clothing also can pose a problem. Sweat, dirt and oils can contribute to acne breakouts, so after an exercise taking a shower is advisable and this should not be delayed. Picking or squeezing blemishes might lead to severe acne scars.
1. I heard hot water kills bacteria and relives acne, should I take a hot shower everyday?
The answer is NO. Hot water does not kill bacteria, however, it can aid clearing the skin pores. At the same time it washes away epidermis own natural secretions which are very protective for your skin. Every-day hot showers could result in over activity of the sebaceous glands by overdrying and depletion of skin lipids and may aggravate acne. Taking a hot bath once a week, maximum twice a week, not more and a cold shower everyday may be helpful. This routine is especially helpful if you exercise. Never leave your skin unwashed after an exercise. Working out your muscle definitely helps your skin by balancing your endocrine system and hormone regulation, which is especially disrupted in hormonaly-induced acne, a mechanism targeted for correction in any protocol for hormonal acne treatment.
In addition it helps your skin by increasing micro circulation of your skin, more generous oxygenation of the stratum corneum and delivery of blood micronutrients essential to combat inflammation and lipid peroxidation, two arresting processes in comedonal acne. Control of inflammation is one of key elements of any approach to treat comedonal acne. Exercise, despite its beneficial effect may turn counterbalancing by providing an environment, open pores, for more readily invasion of bacterial pathogen especially staphylococcus and propionobacterium acnes. During exercise the skin pores open up to allow sweating. After exercise while your skin becomes colder the pores start to close, this is the time all the bacteria on your skin can get inside the closing pores. In normal individuals sebum lipids and epidermal antimicrobial proteins prevent colonization of bacteria but in acne patients these defense mechanisms are apparently compromised.
2. Is this true that an acne-prone skin must use oil-free products?
Being oil free, by itself, does not confer any virtue to a skin care product as a comedonal acne treatment. By the same token, an oily product is not necessarily a bad product. Drying an acne producing skin could be very stimulating for sebaceous glands and their overreaction can make the skin even oilier. This is the scenario when you use a soap to wash your face and body. It is right that high pH of a soap causes overreaction of sebaceous glands, but another stimulation is a dry skin. So the skin should not be over dried. Now, another factor we have to consider is that we have good oils and bad oils. There are pore clogging oils as well as some other oils which benefit the skin in many skin and resemble skin ‘s own natural sebum. Among these oils are jojoba, grape seed oils, rosehip oil, borage oil and many others, These help the skin in one way or another and are not pore-clogging and they should not be considered unwarranted in comedonal acne treatment. What we try to achieve is to treat acne lesions in oily skin to maintain epidermal natural secretions. This maintenance has a regulatory effect on sebaceous gland whose over secretion plays a major part in pathology of acne.>
3. My breakouts become worse during my exam time, anything I can do to help this?
Role of stress and psychological factors has been well established in acne vulgaris and comedone formation. On the other hand psychosomatic impact of acne and burden of the disease make a causal stress effect on acne patients. Stress may trigger hormonal imbalance, corticotropin releasing hormone (CRH) has been suggested as culprit, at pilosebaceous unit and initiates inflammatory mediators involved in pathogenesis of acne.
4. I hear about blackhead removal, should I actually remove a blackhead/whitehead? Does that damage my skin?
The truth is each time a tweezer is used to remove a comedo, a small incision in the skin is produced, which apt to formation of a consequent scarring. This open comedo will be back in a very short time and in some cases might lead to cystic acne, a more severe type of acne, more challenging to treat. However one study in premenstrual acne proposes mild steam to soften comedonal acne and use of enzymatic exfoliation preceding a comedonal extraction in aseptic condition followed by antibacterial and anti inflammatory treatment could be associated with more favorable results. By far evidence for comedonal extraction is lacking and this technique has not been widely accepted in medical practice.
Unlike precedent conceptions, comedones are regarded as inflammatory and comedonal acne treatment should be addressed with this updated view. Comedonal acne treatment starts with an evidence based acne skin care, with keratolytic agents whose clinical efficacy is full proof in eliminating open and closed comedones. In addition, regulating clay based masks could be particularly helpful to relieve various acne lesions in particular comedonal acne. An example is Pore Clarifying Mask. Clay based masks as adjunctive treatment can clear and tighten the pores from inside and balance secretions and concurrently maintain skin oxygenation and regulate inflammation.
5. How about diet and dietary factors, does it have any importance what I eat? Should I avoid certain foods?
Role of diet has spawned a great deal of controversy in medical literature, however, more recent research indicates far more explicitly direct effect of high glycemic index food and dairy products in activating inflammatory processes involved in development of acne vulgaris.
Comedonal acne, long classified under the rubric of “non-inflammatory lesions,” has undergone a conceptual redefinition in recent dermatologic literature. The emerging consensus posits that microcomedones—the incipient lesions in acne vulgaris—are fundamentally inflammatory in nature, thereby challenging the erstwhile dichotomy between comedonal and inflammatory acne. This reframing carries therapeutic implications, as the pathogenesis of comedones is increasingly viewed as a result of subclinical inflammation, follicular hyperkeratinization, dysregulated lipid metabolism, and microbial imbalance.
Effective treatment strategies for comedonal acne must therefore aim beyond the superficial removal of lesions and instead target their etiological core. The elimination of microcomedones remains the central therapeutic goal, as their persistence predicates the development of more advanced inflammatory lesions. The utility of topical agents such as retinoids (e.g., tretinoin, adapalene), beta-hydroxy acids (e.g., salicylic acid), and azelaic acid lies in their ability to normalize keratinocyte desquamation, reduce follicular plugging, and modulate inflammation. Among these, retinoids are the most extensively validated in clinical guidelines as first-line agents for comedonal acne.
Despite a lack of high-grade evidence for some individual agents, evidence-based skin care has gained increasing recognition as a vital adjunct in both exacerbation management and maintenance therapy. Over-the-counter preparations containing benzoyl peroxide, sulfur, or salicylic acid offer benefit in mild disease, yet therapeutic delay is common, with notable improvement often not observed until 6 to 8 weeks of continued application. For patients with moderate to severe disease, or those unresponsive to non-prescription treatments, escalation to prescription regimens involving retinoids, topical antibiotics, and in selected cases, systemic agents, is warranted.
The principle of combination therapy, central to contemporary acne management, underscores the multifaceted nature of the disease. In comedonal acne, however, this principle has been underutilized despite clear pathophysiological justification. Combining keratolytics with antimicrobial agents or anti-inflammatory botanicals not only enhances clinical outcomes but also improves tolerability and reduces potential irritation associated with monotherapy. Notably, benzoyl peroxide and azelaic acid, though only mildly comedolytic, possess antimicrobial and anti-inflammatory properties, which contribute synergistically in multi-agent regimens.
For more severe manifestations such as nodulocystic acne, systemic approaches involving oral antibiotics (e.g., tetracyclines) or isotretinoin are frequently indicated. However, caution is advised given the adverse effect profiles of these agents, including mucocutaneous dryness, teratogenicity, and potential psychological effects. Topical therapies, while not universally curative, remain indispensable in these cases, both as standalone treatments and in adjunct to systemic interventions.
Comedonal acne’s chronicity and tendency toward relapse mandate a proactive approach in maintenance therapy. This involves continuous use of topical agents that not only treat subclinical lesions but also repair the epidermal barrier. The skin-repairing effects of salicylic acid, retinoids, and botanical antioxidants help restore barrier integrity, reduce transepidermal water loss, and protect against environmental insults, thus enhancing patient adherence and long-term disease control.
Preventive strategies are no less crucial. Regular use of non-comedogenic formulations, sun protection, and low-pH cleansers that preserve the acid mantle of the skin are integral to minimizing recurrence. Astringents and soaps, due to their alkalinity, can aggravate sebaceous hyperactivity and microbiome disruption, exacerbating lesion formation. Physical manipulation of comedones—such as picking or extraction—poses a risk for scarring and is discouraged in the absence of clinical indication and aseptic technique.
Emerging research further underscores the interplay between stress, endocrine factors, and acne pathophysiology. Psychoneuroimmunological mechanisms, involving corticotropin-releasing hormone (CRH) and downstream inflammatory cytokines, have been implicated in stress-related flares. Accordingly, stress reduction, exercise, and sleep hygiene are advocated as supportive therapies, with exercise offering additional benefits via improved skin oxygenation, enhanced circulation, and hormonal balance. However, the occlusion and humidity associated with physical activity necessitate timely post-exercise cleansing to prevent bacterial ingress into dilated pores.
The role of diet, once contentious, is gaining empirical support. High glycemic index foods and dairy products have been shown to exacerbate acne through insulin-mediated hormonal shifts and increased androgenic activity, reinforcing the importance of dietary counseling in susceptible individuals.
Lastly, the use of botanically enriched and lipid-regulating skin care regimens represents a burgeoning area of interest. Contrary to traditional avoidance of oils in acne-prone skin, select lipids such as gamma-linolenic acid, rosehip oil, and borage seed oil demonstrate anti-inflammatory and barrier-restorative properties without comedogenicity. These agents may mimic the composition of endogenous sebum, thereby modulating sebaceous gland activity through feedback mechanisms and offering an innovative approach to seborrhea control.
In summary, comedonal acne is increasingly appreciated as a disease of chronic subclinical inflammation, where treatment goals extend beyond lesion resolution to restoration of cutaneous homeostasis. A holistic therapeutic model, integrating evidence-based skin care, pharmacologic intervention, behavioral modification, and dietary regulation, is essential in achieving sustained remission. The evolution of comedonal acne management thus reflects a paradigm shift from lesion eradication to microbiome preservation, barrier support, and patient-centered care.